Main challenges to diagnosing ADHD in females – A narrative review
Marion Risa1, Mai Eline Høiland Selvikvaag1, Marta Maria Gorecka2, Edmund Sonuga-Barke3 & Rune Raudeberg4
1 Department of Biological and Medical Psychology, University of Bergen
2 Department of Psychology, UiT the Arctic University of Norway
3 Department of Child and Adolescent Psychiatry, Institute of Psychiatry, Psychology and Neuroscience, King’s College London
4 Department of Biological and Medical Psychology, University of Bergen
This narrative literature review aimed to investigate factors influencing the identification of ADHD symptoms in girls and women and to propose strategies, developed by the authors based on the reviewed evidence, to address these factors. A search in PubMed, PsycInfo, and Web of Science (WoS), limited to 2021 to 2024, using specific terms related to ADHD and gender differences, yielded 1,729 articles. After removing duplicates and irrelevant articles, 60 were reviewed. Three key factors were identified: (a) caregivers, teachers, and health personnel have insufficient knowledge of gender differences in symptom presentation; (b) differential diagnostic challenges and symptoms overlap; and (c) symptom masking. Our recommendations include: (a) incorporating gender-specific symptom descriptions in ADHD assessment guidelines; (b) recognising that ADHD-related functional impairment is not limited to academic underachievement; and (c) the need for developing better tools to identify and assess symptom masking.
Keywords: attention deficit hyperactivity disorder, ADHD, girls, women, underdiagnosis, misdiagnosis, gender bias
Attention-deficit/hyperactivity disorder (ADHD) affects about 8% of children and adolescents (Ayano, Demelash, et al., 2023) and around 3% of adults (Ayano, Tsegay, et al., 2023). Boys are diagnosed 3–16 times more frequently than girls (Hartung & Lefler, 2019; Nøvik et al., 2006), but in adults the gender ratio varies from 1:1 to 3:1 (Faheem et al., 2022). This suggests that boys are more likely to develop and/or be diagnosed with ADHD or that girls are less likely and/or are underdiagnosed. The differences in gender ratio in adults may in part be attributed to women’s more frequent use of health services overall (Hansen et al., 2012), since contact with health services in adulthood is more dependent on self-referral based on personally experienced symptoms than in childhood, where referral is more dependent on parents and teachers, and where externalising behaviour more prevalent in boys may be the identified behaviour referred.
Women who are first diagnosed with ADHD in adulthood have a higher prevalence of comorbid mental disorders and relational difficulties, and an increased risk of suicide, even when compared to men with ADHD (Babinski, 2024; Kakuszi et al., 2018; C. Skoglund et al., 2024; Williamson & Johnston, 2015). Furthermore, women with ADHD experience higher rates of admission to mental health care compared to women without ADHD, and report more pronounced decline in function compared to men with ADHD (Babinski, 2024; Williamson & Johnston, 2015; Young et al., 2020). Additionally, they face increased risk of financial and occupational difficulties, burnout, and extended sick leave (Fuermaier et al., 2021; Porto et al., 2024). Considering that women with ADHD are diagnosed on average four years later than men (C. Skoglund et al., 2024), early identification of ADHD symptoms is critical for mitigating these adverse outcomes.
In recent years, increased recognition of the existence of ADHD in females has contributed to an increase in referrals and diagnoses. In this article we provide a narrative review of recent studies focused on gender differences in ADHD. We aim to identify factors that might contribute to the delayed assessment and diagnosis of ADHD in girls and women and to propose strategies, developed by the authors based on the reviewed evidence, to address these factors.
Method
We searched in PubMed, PsycInfo and Web of Science (WoS) using: («attention deficit hyperactivity disorder» OR ADHD) AND (girl* OR female* OR women OR «gender difference*« OR «sex difference*« OR «gender gap» OR «gender ratio» OR «sex specific») AND (detection OR identification OR diagnosis* OR screening OR assessment OR examination OR underdiagnosis* OR misdiagnos* OR unrecognise* OR underrepresent*) from 2021 to 2024. Literature reviews, case-control studies, correlation studies, qualitative interview studies, longitudinal studies, cross-sectional studies, prospective cohort studies and retrospective observational studies, as well as relevant comments on published studies, were included. Studies that focused on ADHD symptoms in boys and men only, comorbid disorders rather than ADHD, neurological markers of ADHD and animal studies were excluded. The selection process is illustrated in Figure 1. The final selection was made by the first authors by consensus. During the review process, articles were systematically categorised by method and purpose, and themes identified as conceptually relevant to the research question.
Figure 1
Literature search and selection
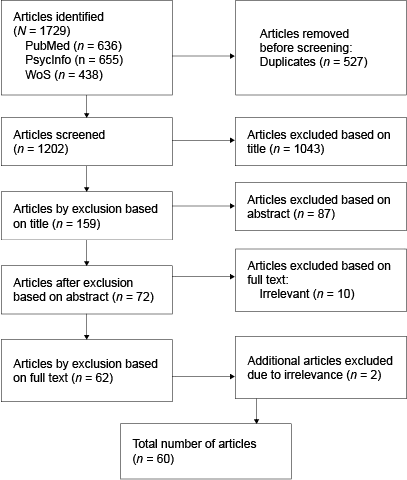
Note. The flow chart shows the number of articles identified, rated, and included or excluded based on predetermined criteria at each stage, from initial search to final selection.
Results
Key themes and subthemes in the selection of articles that highlight obstacles to early detection of ADHD in girls and women are presented in Figure 2. The most important are: (a) differences in symptom presentation, (b) bias in referral and assessment, and (c) differential diagnostic challenges.
Figure 2
Thematic overview of the articles

Note. The figure shows the central themes and subthemes, and the number of articles that discuss the various topics. Some articles discuss several topics, hence the total sum of articles in the flow chart (N = 182) is greater than the number of articles reviewed. The topic ‘Patient Experiences’ is based exclusively on qualitative studies.
Gender differences in symptom presentation
Boys have more symptoms of hyperactivity/impulsivity than girls, while girls have more symptoms of attention difficulties (DuMont et al., 2023; Fraticelli et al., 2022; Hinshaw et al., 2022; Lai et al., 2022; Martin, 2024; Todzia-Kornaś et al., 2024). Boys have more symptoms of oppositional behaviour disorder and more aggression (Mphahlele et al., 2023), while girls have internalised symptoms, such as social withdrawal and depression (Lau et al., 2021). In general, hyperactivity and impulsivity manifest in a more subtle way in girls (Hagstrøm et al., 2024; Hinshaw et al., 2022; Lai et al., 2022; Martin, 2024), and ADHD inattentive subtype is the most common subtype among girls, while boys are more often diagnosed with ADHD combined subtype (Klefsjö et al., 2021; Siddiqui et al., 2024).
Females are older than males when diagnosed with ADHD (Fraticelli et al., 2022; Klefsjö et al., 2021; Martínez-Jaime et al., 2024; Siddiqui et al., 2024; Skoglund et al., 2024). Symptoms of hyperactivity and impulsivity often subside from childhood and into adolescence, especially in boys (Eng et al., 2023; Gilbert et al., 2023), while symptoms of attention difficulties seem to remain stable beyond adolescence, particularly in girls (Eng et al., 2023; Gilbert et al., 2023). ADHD symptoms become more evident and impeding with increasing age in girls as opposed to boys (Lai et al., 2022; Martin, 2024). Destructive behaviours tend to debut in adolescence in girls with ADHD (Hinshaw et al., 2022), and there may be a link between an increase in female sex hormones during puberty and a worsening of ADHD symptoms (Lee et al., 2023; Martin, 2024). Girls and young women with ADHD demonstrate an increased prevalence of sleep disturbances and anxiety symptoms, along with reductions in memory and attentional capacity during menstruation compared to neurotypical peers (Kelly et al., 2024), underscoring the potential influence of fluctuations in female sex hormones on the expression and severity of ADHD symptoms.
In studies that reported no group differences in ADHD symptom profiles between genders, the children were predominantly younger than 13 years of age (De Rossi et al., 2022; Gilbert et al., 2023), and the girls had symptoms of both hyperactivity and inattention, more similar to boys with ADHD (De Rossi et al., 2022; Lynch & Davison, 2024; Siddiqui et al., 2024). Studies in which few (Lin et al., 2023; Loyer Carbonneau et al., 2021) or no gender differences were found (Ceroni et al., 2022; Mphahlele et al., 2022) were based on neuropsychological test results, while those that found the largest gender differences were based on parent and teacher reports (Furzer et al., 2022; Lau et al., 2021; Mphahlele et al., 2023).
Bias in referral and assessment
ADHD is diagnosed more frequently in boys than in girls, even if the symptom presentations are similar (Derks et al., 2007; Ohan & Johnston, 2005; Slobodin & Davidovitch, 2019). Parents and teachers identify more ADHD symptoms in boys (Babinski, 2024; Hinshaw et al., 2022; Olsson, 2023) and consider the extent of ADHD-related difficulties to be greater in boys than in girls, despite the girls themselves reporting greater difficulties than the boys (Andersen et al., 2024). Girls and women must have a higher number of and more severe ADHD symptoms than boys and men before clinicians consider assessment of ADHD (Babinski, 2024; Beheshti et al., 2021; DuMont et al., 2023; Garb, 2021; Hinshaw et al., 2022; Martin, 2024). Women reported that, despite long-term difficulties with concentration and memory, procrastination and poor perception of time, it took a long time before their problems were considered possible symptoms of ADHD (Ginapp et al., 2023; Lynch & Davison, 2024; Mansfield & Soni, 2024; Morley & Tyrrell, 2023). Delayed diagnosis and/or misdiagnosis because the symptom expression did not match the symptoms associated with ADHD in boys seems to be a common experience among women diagnosed with ADHD in adulthood (Ginapp et al., 2023; Lynch & Davison, 2024; Morgan, 2023; Morley & Tyrrell, 2023). The results indicate that gender stereotypes influence the identification and treatment of ADHD symptoms.
Comorbidity and differential diagnostic challenges
Girls and women are frequently diagnosed with other conditions before they are diagnosed with ADHD (Kelly et al., 2024; Klefsjö et al., 2021; Lai et al., 2022; Siddiqui et al., 2024). Girls and women with ADHD are about twice as likely as boys and men with ADHD to be diagnosed with anxiety and depression (Quinn, 2008; C. Skoglund et al., 2024), and are more often treated for these disorders before being assessed for ADHD (Ginapp et al., 2023; Long & Coats, 2022; Lynch & Davison, 2024; Morgan, 2023). Several studies indicate that anxiety and depression can be secondary to (untreated) ADHD in females (Ahmad et al., 2021; Attoe & Climie, 2023; Ginapp et al., 2023; Long & Coats, 2022; Morgan, 2023; Morley & Tyrrell, 2023), and that the symptoms of these disorders can overshadow underlying ADHD (Blikø, 2008; Taylor et al., 2019). In qualitative studies, a common finding is that treatment for anxiety and/or depression had little or no effect but that symptoms decreased or disappeared after starting on ADHD medication (Ginapp et al., 2023; Morgan, 2023). In addition, borderline personality disorder and bipolar disorder type II have symptoms (especially emotional dysregulation and hyperactivity) that overlap with ADHD (Moukhtarian et al., 2021; Comparelli et al., 2022), making clinical assessment challenging.
Emotional dysregulation is common among both boys and girls with ADHD (De Ronda et al., 2024; Kahle et al., 2021; Welkie et al., 2021). While these difficulties tend to diminish with age in boys, they often persist or worsen in girls and in those with subclinical symptoms (De Ronda et al., 2024; Gilbert et al., 2023). This may increase girls’ vulnerability to depression and anxiety over time due to sustained emotional dysregulation (De Ronda et al., 2024; Gilbert et al., 2023; Welkie et al., 2021). Moreover, some evidence suggests that emotional dysregulation can serve as an indicator of underlying ADHD (Kahle et al., 2021).
Females with ADHD have a more complex and severe symptom constellation when the ADHD diagnosis is first made (Babinski, 2024; Hinshaw et al., 2022), and have a higher risk of developing substance abuse problems and earlier onset of unsafe sexual behaviour compared to males with ADHD (Castellano-García et al., 2022; El Rasheed et al., 2023; Lai et al., 2022). Furthermore, women with ADHD have a higher risk of self-harm and suicide attempts compared to men with ADHD (Hinshaw et al., 2022; O’Grady & Hinshaw, 2021; C. Skoglund et al., 2024; Todzia-Kornaś et al., 2024; Ward & Curran, 2021).
Masking ADHD symptoms
Trying to hide and/or compensating for ADHD symptoms (i.e., masking) is prevalent among girls and women with ADHD (Ceroni et al., 2022; DuMont et al., 2023; Hinshaw et al., 2022; Kelly et al., 2024; Lai et al., 2022; Martin, 2024; Wicherkiewicz & Gambin, 2024). The purpose of masking is to better meet social expectations, avoid negative attention, and to fit in better socially. For instance, in ADHD, it can involve overpreparing, checking, and appearing attentive (Bürger et al., 2024; Ginapp et al., 2023; Long & Coats, 2022; Mansfield & Soni, 2024; Morgan, 2023; Morley & Tyrrell, 2023; Pearson & Rose, 2021). Girls with ADHD use compensatory strategies to a greater extent than boys with ADHD (Hinshaw et al., 2022; Lai et al., 2022; Martin, 2024; Wicherkiewicz & Gambin, 2024), but prolonged masking increases the risk of low self-esteem, burnout, anxiety and depression, since masking requires lots of energy and affects one’s sense of self and identity (Wicherkiewicz & Gambin, 2024). It should be noted that adolescent girls in general use masking or compensation as a social adaptation strategy, but in girls with ADHD its intensity and consequences differ in that masking requires more mental effort, leading to more fatigue and stress, and reducing cognitive resources for learning and social interaction (McKinney et al., 2024).
Discussion
The purpose of this literature review was to investigate whether factors can be identified that may delay the diagnosis of girls with ADHD and to propose strategies, based on the reviewed evidence, to address these factors. The results indicate that girls’ symptoms of ADHD are dominated by attention difficulties (Fraticelli et al., 2022; Siddiqui et al., 2024; C. Skoglund et al., 2024), and that they have less hyperactivity and impulsivity (Hagstrøm et al., 2024; Lai et al., 2022; Martin, 2024). Gender differences in symptom expression can lead to girls’ ADHD symptoms being overlooked or underestimated (Hinshaw et al., 2022; Lai et al., 2022) or perceived as another condition, most often as anxiety and/or depression (Quinn, 2008; C. Skoglund et al., 2024). In qualitative studies, masking is highlighted as a major reason why ADHD symptoms were not detected or not understood (Mansfield & Soni, 2024; Morley & Tyrrell, 2023). Because ADHD symptoms seem to worsen for many girls during puberty (Mansfield & Soni, 2024; Morley & Tyrrell, 2023), at a time when demands for independence increase beyond adolescence and into young adulthood, it becomes more difficult to mask symptoms (Lai et al., 2022; Martin, 2024). Thus, symptoms appear to debut in adulthood and ADHD becomes a less plausible diagnosis, given that one criterion for the diagnosis is that symptoms must be present before the age of 12 (American Psychiatric Association, 2013).
The assumption that girls and women with ADHD are underdiagnosed is challenged by statistics showing that the proportion of girls with an ADHD diagnosis has increased markedly. Data from the Norwegian Public Health Report showed that registered ADHD diagnoses in young women (16–19 years) doubled from 1.5% in 2019 to 3.1% in 2022, far greater than for boys in the same age range in the same period (Bang et al., 2024). However, in 2022 there were still 2.5 times more boys than girls in the age group 6–11 years registered with an ADHD diagnosis, and a total of 38% more boys and men with an ADHD diagnosis was registered for the period 2010–2022 (Bang et al., 2024). It is possible that some of the increased prevalence of ADHD observed in boys compared to girls can be explained by a greater vulnerability in boys to developing ADHD, but this is still unclear (Arnett et al., 2015; Camara et al., 2022). Overall, there is still reason to be aware of factors that may contribute to delayed diagnosis in girls.
Interventions that can promote earlier detection and diagnosis
Official guidelines for the assessment of ADHD highlight that girls are probably underdiagnosed (Norwegian Directorate of Health, 2022; National Institute for Health and Care Excellence, 2018). DSM-5 briefly mentions that girls and women primarily have attention difficulties (American Psychiatric Association, 2013), but provides no descriptions of gender differences in symptom expression, such as that hyperactivity in girls often consists of racing thoughts, inner restless and/or agitation, and excessive talking (Hagstrøm et al., 2024; Hinshaw et al., 2022; Lai et al., 2022; Martin, 2024). Including gender-specific examples of symptom expressions in diagnostic manuals and guidelines can help identify more girls with ADHD. Another possibility is to require a smaller number of symptoms for girls than for boys (Olofsdotter et al., 2023). However, this may give the impression that girls and women have a less severe form of ADHD and does not solve the original problem, which is that the symptom assessment forms are best at measuring hyperactivity (Hagstrøm et al., 2024). A better solution would be to develop assessment instruments aimed at better at identifying ADHD symptoms that are typical for girls. For example, emotional dysregulation in ADHD may manifest as behaviours such as excessive apologising and heightened guilt responses, which are not captured by traditional symptom checklists (Platania et al., 2025).
Diagnostic overshadowing and comorbidity contribute to the misdiagnosis of girls and women with ADHD (Babinski, 2024; Ginapp et al., 2023; Hinshaw et al., 2022). Increased knowledge about diagnostic overshadowing helps to ensure that more people can receive the right treatment earlier and prevent the development of comorbidity. Self-harm, unsafe sexual activity and substance abuse can be expressions of hyperactivity and impulsivity, thus indicating ADHD (El Rasheed et al., 2023; Todzia-Kornaś et al., 2024; Ward & Curran, 2021). At the same time, the relationships between these conditions and/or symptoms are understudied, undercommunicated and poorly understood (L. B. Skoglund, 2024). Moreover, there is a lack of knowledge about whether, or how, sex hormones affect the onset of ADHD, the severity of ADHD symptoms, and the effect of ADHD medication in women (Bürger et al., 2024).
A necessary criterion for the diagnosis is that the ADHD symptoms lead to functional impairment. According to DSM-5 (American Psychiatric Association, 2013), functional loss in childhood manifests as decreased school performance and social rejection, and in adulthood as problems in working life and increased interpersonal conflicts. However, many girls who were diagnosed late did not perform poorly in school or had externalisation difficulties in childhood (Mansfield & Soni, 2024; Morley & Tyrrell, 2023). Many reported having spent an excessive amount of time on schoolwork, planning and organising to compensate for their difficulties (Lynch & Davison, 2024; Morgan, 2023). Masking of ADHD symptoms is probably one of the most important reasons why girls and women with ADHD are diagnosed late and/or misdiagnosed. There is a lack of knowledge about masking ADHD symptoms, and such knowledge would be useful to better understand which compensatory strategies are used to mask symptoms, and how masking could be assessed as part of a diagnostic process. Research on masking in autism, such as the development and use of the Camouflaging Autistic Traits Questionnaire (CAT-Q; Hull et al., 2019), may provide valuable insights and methodological approaches for studying masking in ADHD. Recent advances in machine learning and artificial intelligence have demonstrated that it is possible to develop diagnostic algorithms that can either perpetuate or mitigate gender bias (Neufang et al., 2025), but further development and validation are needed for clinical application. More research on ADHD symptoms from a life-course perspective seems particularly relevant to better understand ADHD symptoms in adolescents and young adult women and how their symptoms differ and/or develop at different ages.
Although the scope of this review was the underdiagnosis of females with ADHD, we acknowledge that boys with mainly inattentive symptoms, may also be underdetected due to gender-atypical symptom presentation and masking. This topic should be addressed in future studies.
Limitations
The flexible, non-standardised methodology for article selection makes it difficult for others to replicate this study, and the absence of clearly defined frameworks for the selection and analysis of studies, combined with subjective assessments and interpretations, can lead to selection and interpretation bias. It cannot be ruled out that studies and results that fit with our assumptions and perspectives have been highlighted to a greater extent than other studies. We did not track which references were retrieved through the systematic search versus those added later for context. While all cited studies are relevant to the research question, future reviews should explicitly document this distinction to enhance transparency and reproducibility. For reasons of brevity, we have not included other important obstacles, such as low socioeconomic status or lack of capacity in the specialist health care service.
The ADHD concept has been operationalised and assessed in different ways in the included studies, making it difficult to compare results. Many of the included studies have several methodological weaknesses that affect the evidence base for our conclusions. Since we have not systematically assessed quality, studies of high quality and with stronger evidence were not necessarily given more weight than studies of weaker quality.
Conclusion
Although a larger proportion of girls and women is diagnosed with ADHD today than 10 years ago (Bang et al., 2024), the results of this literature review indicate that there is still a need to increase the understanding of gender-related differences in ADHD symptoms. This study shows that differences in symptom presentation, bias in referral and understanding of symptoms, and comorbidity and masking/compensation are central in ADHD in women. Increased knowledge about gender differences in symptom expression, masking of symptoms, and diagnostic overshadowing will help to ensure that more girls with ADHD are identified, examined and diagnosed, and receive appropriate and necessary health care earlier.
References
Ahmad, S. I., Meza, J. I., Posserud, M.-B., Brevik, E. J., Hinshaw, S. P., & Lundervold, A. J. (2021). Attention-Deficit/Hyperactivity Disorder Symptom Dimensions Differentially Predict Adolescent Peer Problems: Findings from Two Longitudinal Studies. Frontiers in Psychology, 11, 609 789. https://doi.org/10.3389/fpsyg.2020.609 789
American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
Andersen, A. C., Sund, A. M., Thomsen, P. H., Lydersen, S., Haugan, A.-L. J., & Nøvik, T. S. (2024). Executive function measured by BRIEF in adolescents diagnosed and treated for ADHD: Problem profiles and agreement between informants. Child Neuropsychology, 30(1), 45–59. https://doi.org/10.1080/09 297 049.2023.2 174 506
Arnett, A. B., Pennington, B. F., Willcutt, E. G., DeFries, J. C., & Olson, R. K. (2015). Sex differences in ADHD symptom severity. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 56(6), 632–639. https://doi.org/10.1111/jcpp.12337
Attoe, D. E., & Climie, E. A. (2023). Miss. Diagnosis: A Systematic Review of ADHD in Adult Women. Journal of Attention Disorders, 27(7), 645–657. https://doi.org/10.1177/10 870 547 231 161 533
Ayano, G., Demelash, S., Gizachew, Y., Tsegay, L., & Alati, R. (2023). The global prevalence of attention deficit hyperactivity disorder in children and adolescents: An umbrella review of meta-analyses. Journal of Affective Disorders, 339, 860–866. https://doi.org/10.1016/j.jad.2023.07.071
Ayano, G., Tsegay, L., Gizachew, Y., Necho, M., Yohannes, K., Abraha, M., Demelash, S., Anbesaw, T., & Alati, R. (2023). Prevalence of attention deficit hyperactivity disorder in adults: Umbrella review of evidence generated across the globe. Psychiatry Research, 328, 115 449. https://doi.org/10.1016/j.psychres.2023.115 449
Babinski, D. E. (2024). Sex Differences in ADHD: Review and Priorities for Future Research. Current Psychiatry Reports, 26(4), 151–156. https://doi.org/10.1007/s11 920–024–01 492–6
Bang, L., Furu, K., Handal, M., Torgersen, L., Stavenes Støle, H., Surén, P., Odsbu, I., & Hartz, I. (2024). Folkehelserapporten. Psykiske plager og lidelser hos barn og unge [The public health report Mental ailments and disorders in children and adolescents]. https://www.fhi.no/he/folkehelserapporten/psykisk-helse/psykisk-helse-hos-barn-og-unge/?term=
Beheshti, A., Chavanon, M.-L., Schneider, S., & Christiansen, H. (2021). ADHD overdiagnosis and the role of patient gender among Iranian psychiatrists. BMC Psychiatry, 21(1), 514. https://doi.org/10.1186/s12 888–021–03 525–3
Blikø, I. K. K. (2008). ADHD hos voksne: En undersøkelse av diagnostikk, komorbiditet og problembelastning [ADHD in adults: An examination of diagnostics, comorbidity and problem loading]. Tidsskrift for Norsk psykologforening, 45(5), 536–544. https://www.psykologtidsskriftet.no/artikkel/2008as04ae-ADHD-hos-voksne-En-undersokelse-av-diagnostikk-komorbiditet-og-problembelastning
Bürger, I., Erlandsson, K., & Borneskog, C. (2024). Perceived associations between the menstrual cycle and Attention Deficit Hyperactivity Disorder (ADHD): A qualitative interview study exploring lived experiences. Sexual & Reproductive Healthcare, 40, 100 975. https://doi.org/10.1016/j.srhc.2024.100 975
Camara, B., Padoin, C., & Bolea, B. (2022). Relationship between sex hormones, reproductive stages and ADHD: A systematic review. Archives of Women’s Mental Health, 25(1), 1–8. https://doi.org/10.1007/s00 737–021–01 181-w
Castellano-García, F., Benito, A., Jovani, A., Fuertes-Sáiz, A., Marí-Sanmillán, M. I., & Haro, G. (2022). Sex Differences in Substance Use, Prevalence, Pharmacological Therapy, and Mental Health in Adolescents with Attention-Deficit/Hyperactivity Disorder (ADHD). Brain Sciences, 12(5), 590. https://doi.org/10.3390/brainsci12 050 590
Ceroni, M., Rossi, S., Zerboni, G., Biglia, E., Soldini, E., Izzo, A., Morellini, L., & Sacco, L. (2022). Attentive-executive functioning and compensatory strategies in adult ADHD: A retrospective case series study. Frontiers in Psychology, 13, 1 015 102. https://doi.org/10.3389/fpsyg.2022.1 015 102
Comparelli, A., Polidori, L., Sarli, G., Pistollato, A., & Pompili, M. (2022). Differentiation and comorbidity of bipolar disorder and attention deficit and hyperactivity disorder in children, adolescents, and adults: A clinical and nosological perspective. Frontiers in Psychiatry, 13, 949 375. https://doi.org/10.3389/fpsyt.2022.949 375
De Ronda, A. C., Rice, L., Zhao, Y., Rosch, K. S., Mostofsky, S. H., & Seymour, K. E. (2024). ADHD-related sex differences in emotional symptoms across development. European Child & Adolescent Psychiatry, 33(5), 1419–1432. https://doi.org/10.1007/s00 787–023–02 251–3
De Rossi, P., Pretelli, I., Menghini, D., D’Aiello, B., Di Vara, S., & Vicari, S. (2022). Gender-Related Clinical Characteristics in Children and Adolescents with ADHD. Journal of Clinical Medicine, 11(2), 385. https://doi.org/10.3390/jcm11 020 385
Derks, E. M., Hudziak, J. J., & Boomsma, D. I. (2007). Why More Boys Than Girls With ADHD Receive Treatment: A Study of Dutch Twins. Twin Research and Human Genetics, 10(5), 765–770. https://doi.org/10.1375/twin.10.5.765
DuMont, M., Agostinis, A., Singh, K., Swan, E., Buttle, Y., & Tropea, D. (2023). Sex representation in neurodegenerative and psychiatric disorders’ preclinical and clinical studies. Neurobiology of Disease, 184, 106 214. https://doi.org/10.1016/j.nbd.2023.106 214
El Rasheed, A. H., Abd El Moneam, M. H. E.-D., Tawfik, F., Farid, R. W. M., & Elrassas, H. (2023). Risk behaviors in substance use disorder in a sample of Egyptian female patients with or without symptoms of attention-deficit hyperactivity disorder. Middle East Current Psychiatry, 30(1), 18. https://doi.org/10.1186/s43 045–023–00 295–4
Eng, A. G., Phan, J. M., Shirtcliff, E. A., Eisenlohr-Moul, T. A., Goh, P. K., & Martel, M. M. (2023). Aging and Pubertal Development Differentially Predict Symptoms of ADHD, Depression, and Impairment in Children and Adolescents: An Eight-Year Longitudinal Study. Research on Child and Adolescent Psychopathology, 51(6), 819–832. https://doi.org/10.1007/s10 802–023–01 030–7
Faheem, M., Akram, W., Akram, H., Khan, M. A., Siddiqui, F. A., & Majeed, I. (2022). Gender-based differences in prevalence and effects of ADHD in adults: A systematic review. Asian Journal of Psychiatry, 75, 103 205. https://doi.org/10.1016/j.ajp.2022.103 205
Fraticelli, S., Caratelli, G., De Berardis, D., Ducci, G., Pettorruso, M., Martinotti, G., Di Cesare, G., & di Giannantonio, M. (2022). Gender differences in attention deficit hyperactivity disorder: An update of the current evidence. Rivista Di Psichiatria, 57(4), 159–164. https://doi.org/10.1708/3855.38 380
Fuermaier, A. B. M., Tucha, L., Butzbach, M., Weisbrod, M., Aschenbrenner, S., & Tucha, O. (2021). ADHD at the workplace: ADHD symptoms, diagnostic status, and work-related functioning. Journal of Neural Transmission, 128(7), 1021–1031. https://doi.org/10.1007/s00 702–021–02 309-z
Furzer, J., Dhuey, E., & Laporte, A. (2022). ADHD misdiagnosis: Causes and mitigators. Health Economics, 31(9), 1926–1953. https://doi.org/10.1002/hec.4555
Garb, H. N. (2021). Race bias and gender bias in the diagnosis of psychological disorders. Clinical Psychology Review, 90, 102 087. https://doi.org/10.1016/j.cpr.2021.102 087
Gilbert, M., Boecker, M., Reiss, F., Kaman, A., Erhart, M., Schlack, R., Westenhöfer, J., Döpfner, M., & Ravens-Sieberer, U. (2023). Gender and Age Differences in ADHD Symptoms and Co-occurring Depression and Anxiety Symptoms Among Children and Adolescents in the BELLA Study. Child Psychiatry & Human Development. https://doi.org/10.1007/s10 578–023–01 622-w
Ginapp, C. M., Greenberg, N. R., MacDonald-Gagnon, G., Angarita, G. A., Bold, K. W., & Potenza, M. N. (2023). «Dysregulated not deficit»: A qualitative study on symptomatology of ADHD in young adults. PLOS ONE, 18(10), e0 292 721. https://doi.org/10.1371/journal.pone.0 292 721
Hagstrøm, J., Nielsen, T., Sørensen, M. E., Aagaard, K., Arendt Rasmussen, M., Rosenberg, J. B., Mohammadzadeh, P., Sevelsted, A., Hernández-Lorca, M., Fagerlund, B., Rydkjær, J., Pagsberg, A. K., Kaufman, J., Ebdrup, B. H., Bilenberg, N., & Jepsen, J. R. M. (2024). Dimensional profiling of psychopathology in children and adolescents based on the K-SADS-PL and an analysis of the construct validity of two ADHD symptom dimensions. Nordic Journal of Psychiatry, 78(1), 71–78. https://doi.org/10.1080/08 039 488.2023.2 262 997
Hansen, A. H., Halvorsen, P. A., Ringberg, U., & Førde, O. H. (2012). Socio-economic inequalities in health care utilisation in Norway: A population based cross-sectional survey. BMC Health Services Research, 12(1), 336. https://doi.org/10.1186/1472–6963–12–336
Hartung, C. M., & Lefler, E. K. (2019). Sex and gender in psychopathology: DSM–5 and beyond. Psychological Bulletin, 145(4), 390–409. https://doi.org/10.1037/bul0 000 183
Hinshaw, S. P., Nguyen, P. T., O’Grady, S. M., & Rosenthal, E. A. (2022). Annual Research Review: Attention‐deficit/hyperactivity disorder in girls and women: underrepresentation, longitudinal processes, and key directions. Journal of Child Psychology and Psychiatry, 63(4), 484–496. https://doi.org/10.1111/jcpp.13 480
Hull, L., Mandy, W., Lai, M.-C., Baron-Cohen, S., Allison, C., Smith, P., & Petrides, K. V. (2019). Development and Validation of the Camouflaging Autistic Traits Questionnaire (CAT-Q). Journal of Autism and Developmental Disorders, 49(3), 819–833. https://doi.org/10.1007/s10803-018-3792-6
Kahle, S., Mukherjee, P., Dixon, J. F., Leibenluft, E., Hinshaw, S. P., & Schweitzer, J. B. (2021). Irritability Predicts Hyperactive/Impulsive Symptoms Across Adolescence for Females. Research on Child and Adolescent Psychopathology, 49(2), 185–196. https://doi.org/10.1007/s10 802–020–00 723–7
Kakuszi, B., Bitter, I., & Czobor, P. (2018). Suicidal ideation in adult ADHD: Gender difference with a specific psychopathological profile. Comprehensive Psychiatry, 85, 23–29. https://doi.org/10.1016/j.comppsych.2018.06.003
Kelly, C., Martin, R., Taylor, R., & Doherty, M. (2024). Recognising and responding to physical and mental health issues in neurodivergent girls and women. British Journal of Hospital Medicine, 85(4), 1–12. https://doi.org/10.12 968/hmed.2023.0337
Klefsjö, U., Kantzer, A. K., Gillberg, C., & Billstedt, E. (2021). The road to diagnosis and treatment in girls and boys with ADHD – gender differences in the diagnostic process. Nordic Journal of Psychiatry, 75(4), 301–305. https://doi.org/10.1080/08 039 488.2020.1 850 859
Lai, M.-C., Lin, H.-Y., & Ameis, S. H. (2022). Towards equitable diagnoses for autism and attention-deficit/hyperactivity disorder across sexes and genders. Current Opinion in Psychiatry, 35(2), 90–100. https://doi.org/10.1097/YCO.0 000 000 000 000 770
Lau, T. W. I., Lim, C. G., Acharryya, S., Lim-Ashworth, N., Tan, Y. R., & Fung, S. S. D. (2021). Gender differences in externalizing and internalizing problems in Singaporean children and adolescents with attention-deficit/hyperactivity disorder. Child and Adolescent Psychiatry and Mental Health, 15(1), 3. https://doi.org/10.1186/s13 034–021–00 356–8
Lee, J., Lee, S. I., Lee, Y. M., & Hong, Y. H. (2023). Prevalence of Attention Deficit Hyperactivity Disorder in Girls With Central Precocious Puberty. Journal of Attention Disorders, 27(13), 1460–1466. https://doi.org/10.1177/10 870 547 231 180 116
Lin, H.-Y., Chiu, E.-C., Hsieh, H.-C., & Wang, P.-J. (2023). Gender Differences in Auditory and Visual Attentional Performance in Children with and without ADHD. Archives of Clinical Neuropsychology, 38(6), 891–903. https://doi.org/10.1093/arclin/acad019
Long, N., & Coats, H. (2022). The need for earlier recognition of attention deficit hyperactivity disorder in primary care: A qualitative meta-synthesis of the experience of receiving a diagnosis of ADHD in adulthood. Family Practice, 39(6), 1144–1155. https://doi.org/10.1093/fampra/cmac038
Loyer Carbonneau, M., Demers, M., Bigras, M., & Guay, M.-C. (2021). Meta-Analysis of Sex Differences in ADHD Symptoms and Associated Cognitive Deficits. Journal of Attention Disorders, 25(12), 1640–1656. https://doi.org/10.1177/1 087 054 720 923 736
Lynch, A., & Davison, K. (2024). Gendered expectations on the recognition of ADHD in young women and educational implications. Irish Educational Studies, 43(1), 61–81. https://doi.org/10.1080/03 323 315.2022.2 032 264
Mansfield, E. M. G., & Soni, A. (2024). ‘I have it, so I understand it, I feel it’: The secondary school experiences of adolescent females with ADHD in England. Journal of Research in Special Educational Needs, 24(3), 681–695. https://doi.org/10.1111/1471–3802.12 660
Martin, J. (2024). Why are females less likely to be diagnosed with ADHD in childhood than males? The Lancet Psychiatry, 11(4), 303–310. https://doi.org/10.1016/S2215–0366(24)00 010–5
Martínez-Jaime, M. M., Reyes-Morales, H., Peyrot-Negrete, I., & Barrientos-Álvarez, M. S. (2024). Access to early diagnosis for attention-deficit/hyperactivity disorder among children and adolescents in Mexico City at specialized mental health services. BMC Health Services Research, 24(1), 599. https://doi.org/10.1186/s12 913–024–11 022-y
McKinney, A., O’Brien, S., Maybin, J. A., Chan, S. W. Y., Richer, S., & Rhodes, S. (2024). Camouflaging in neurodivergent and neurotypical girls at the transition to adolescence and its relationship to mental health: A participatory methods research study. JCPP advances, 4(4), e12 294. https://doi.org/10.1002/jcv2.12 294
Morgan, J. (2023). Exploring women’s experiences of diagnosis of ADHD in adulthood: A qualitative study. Advances in Mental Health, 1–15. https://doi.org/10.1080/18 387 357.2023.2 268 756
Morley, E., & Tyrrell, A. (2023). Exploring Female Students’ Experiences of ADHD and its Impact on Social, Academic, and Psychological Functioning. Journal of Attention Disorders, 27(10), 1129–1155. https://doi.org/10.1177/10 870 547 231 168 432
Moukhtarian, T. R., Reinhard, I., Moran, P., Ryckaert, C., Skirrow, C., Ebner-Priemer, U., & Asherson, P. (2021). Comparable emotional dynamics in women with ADHD and borderline personality disorder. Borderline personality disorder and emotion dysregulation, 8(1), 6. https://doi.org/10.1186/s40 479–021–00 144-y
Mphahlele, R. M., Meyer, A., & Pillay, B. J. (2022). Working memory and set-shifting in school-aged children classified as having attention-deficit hyperactivity disorder. South African Journal of Psychiatry, 28. https://doi.org/10.4102/sajpsychiatry.v28i0.1729
Mphahlele, R. M., Pillay, B. J., & Meyer, A. (2023). Symptoms of oppositional defiant disorder, conduct disorder and anger in children with ADHD. South African Journal of Education, 43(1), 1–14. https://doi.org/10.15 700/saje.v43n1a2136
National Institute for Health and Care Excellence. (2018, mai 14). Attention deficit hyperactivity disorder: Diagnosis and management (NICE guideline NG87). NICE National Institute for Health and Care Excellence. https://www.nice.org.uk/guidance/ng87
Neufang, S., Li, F., Akhrif, A., & Beyan, O. D. (2025). Toward a fair, gender-debiased classifier for the diagnosis of attention deficit/hyperactivity disorder- a Machine-Learning based classification study. BMC medical informatics and decision making, 25(1), 290. https://doi.org/10.1186/s12 911–025–03 126–0
Norwegian Directorate of Health. (2022). ADHD/Hyperkinetisk forstyrrelse – Nasjonal faglig retningslinje for utredning, behandling og oppfølging [ADHD/Hyperkinetic Disorder – National professional guidelines for assessment, treatment and follow-up]. https://www.helsedirektoratet.no/retningslinjer/adhd
Nøvik, T. S., Hervas, A., Ralston**, S. J., Dalsgaard, S., Rodrigues Pereira, R., Lorenzo, M. J., & ADORE Study Group*. (2006). Influence of gender on Attention-Deficit/Hyperactivity Disorder in Europe – ADORE. European Child & Adolescent Psychiatry, 15(S1), i15–i24. https://doi.org/10.1007/s00 787–006–1003-z
O’Grady, S. M., & Hinshaw, S. P. (2021). Long-term outcomes of females with attention-deficit hyperactivity disorder: Increased risk for self-harm. The British Journal of Psychiatry, 218(1), 4–6. https://doi.org/10.1192/bjp.2020.153
Ohan, J. L., & Johnston, C. (2005). Gender Appropriateness of Symptom Criteria for Attention-Deficit/Hyperactivity Disorder, Oppositional-Defiant Disorder, and Conduct Disorder. Child Psychiatry and Human Development, 35(4), 359–381. https://doi.org/10.1007/s10578-005-2694-y
Olofsdotter, S., Fernández-Quintana, Á., Sonnby, K., & Vadlin, S. (2023). Clinical utility of new cut-off scores for the world health organization ADHD self-report scale among adolescents in psychiatric outpatient care. International Journal of Clinical and Health Psychology, 23(4), 100 391. https://doi.org/10.1016/j.ijchp.2023.100391
Olsson, Å. (2023). Teachers’ gendered perceptions of attention deficit hyperactivity disorder – a literature review. European Journal of Special Needs Education, 38(3), 303–316. https://doi.org/10.1080/08 856 257.2022.2 076 476
Platania, N. M., Starreveld, D. E. J., Wynchank, D., Beekman, A. T. F., & Kooij, S. (2025). Bias by gender: exploring gender-based differences in the endorsement of ADHD symptoms and impairment among adult patients. Frontiers in global women’s health, 6, 1 549 028. https://doi.org/10.3389/fgwh.2025.1 549 028
Porto, T. I., Murgo, C. S., & Souza, A. P. D. (2024). Prevalence and Correlations Between ADHD and Burnout Dimensions in Brazilian University Students. Paidéia (Ribeirão Preto), 34, e3413. https://doi.org/10.1590/1982–4327e3413
Quinn, P. O. (2008). Attention-deficit/hyperactivity disorder and its comorbidities in women and girls: An evolving picture. Current Psychiatry Reports, 10(5), 419–423. https://doi.org/10.1007/s11 920–008–0067–5
Siddiqui, U., Conover, M. M., Voss, E. A., Kern, D. M., Litvak, M., & Antunes, J. (2024). Sex Differences in Diagnosis and Treatment Timing of Comorbid Depression/Anxiety and Disease Subtypes in Patients With ADHD: A Database Study. Journal of Attention Disorders, 28(10), 1347–1356. https://doi.org/10.1177/10 870 547 241 251 738
Skoglund, C., Sundström Poromaa, I., Leksell, D., Ekholm Selling, K., Cars, T., Giacobini, M., Young, S., & Kopp Kallner, H. (2024). Time after time: Failure to identify and support females with ADHD – a Swedish population register study. Journal of Child Psychology and Psychiatry, 65(6), 832–844. https://doi.org/10.1111/jcpp.13 920
Skoglund, L. B. (2024). ADHD Girls to Women: Getting on the Radar. Jessica Kingsley Publishers. ISBN: 9 781 805 010 548.
Slobodin, O., & Davidovitch, M. (2019). Gender Differences in Objective and Subjective Measures of ADHD Among Clinic-Referred Children. Frontiers in Human Neuroscience, 13, 441. https://doi.org/10.3389/fnhum.2019.00441
Taylor, M. J., Lichtenstein, P., Larsson, H., Anckarsäter, H., Greven, C. U., & Ronald, A. (2016). Is There a Female Protective Effect Against Attention-Deficit/Hyperactivity Disorder? Evidence From Two Representative Twin Samples. Journal of the American Academy of Child & Adolescent Psychiatry, 55(6), 504–512.e2. https://doi.org/10.1016/j.jaac.2016.04.004
Taylor, M. J., Larsson, H., Gillberg, C., Lichtenstein, P., & Lundström, S. (2019). Investigating the childhood symptom profile of community‐based individuals diagnosed with attention‐deficit/hyperactivity disorder as adults. Journal of Child Psychology and Psychiatry, 60(3), 259–266. https://doi.org/10.1111/jcpp.12988
Todzia-Kornaś, A., Szczegielniak, A., & Gondek, T. M. (2024). Suicidality and nonsuicidal self-injury in females diagnosed with attention-deficit hyperactivity disorder—A narrative review. Current Opinion in Psychiatry, 37(1), 38–42. https://doi.org/10.1097/YCO.0 000 000 000 000 908
Ward, J. H., & Curran, S. (2021). Self‐harm as the first presentation of attention deficit hyperactivity disorder in adolescents. Child and Adolescent Mental Health, 26(4), 303–309. https://doi.org/10.1111/camh.12 471
Welkie, J., Babinski, D. E., & Neely, K. A. (2021). Sex and Emotion Regulation Difficulties Contribute to Depression in Young Adults With Attention-Deficit/Hyperactivity Disorder. Psychological Reports, 124(2), 596–610. https://doi.org/10.1177/0 033 294 120 918 803
Wicherkiewicz, F., & Gambin, M. (2024). Relations Between Social Camouflaging, Life Satisfaction, and Depression Among Polish Women with ADHD. Journal of Autism and Developmental Disorders. https://doi.org/10.1007/s10 803–024–06 410–6
Williamson, D., & Johnston, C. (2015). Gender differences in adults with attention-deficit/hyperactivity disorder: A narrative review. Clinical Psychology Review, 40, 15–27. https://doi.org/10.1016/j.cpr.2015.05.005
Young, S., Adamo, N., Ásgeirsdóttir, B. B., Branney, P., Beckett, M., Colley, W., Cubbin, S., Deeley, Q., Farrag, E., Gudjonsson, G., Hill, P., Hollingdale, J., Kilic, O., Lloyd, T., Mason, P., Paliokosta, E., Perecherla, S., Sedgwick, J., Skirrow, C., … Woodhouse, E. (2020). Females with ADHD: An expert consensus statement taking a lifespan approach providing guidance for the identification and treatment of attention-deficit/ hyperactivity disorder in girls and women. BMC Psychiatry, 20(1), 404. https://doi.org/10.1186/s12 888–020–02 707–9
